
September 13: National Celiac Disease Awareness Day
Each year, September 13 marks National Celiac Disease Awareness Day, a time dedicated to increasing understanding and awareness of the impact celiac disease can have on individuals. Following the recent national holiday, TSF is highlighting celiac disease, as it is more common in individuals with Turner syndrome (TS) (Mårild et al., 2016).
This article will explore what celiac disease is, why it occurs, and common symptoms. It will also explain how to get diagnosed, discuss treatment options, and address the unique challenges faced by individuals with both Turner syndrome and celiac disease.
What is Celiac Disease?
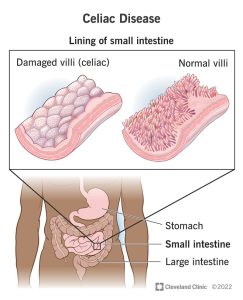
Celiac disease is an autoimmune disorder where the ingestion of gluten – a protein found in wheat, barley, and rye – triggers an immune response that damages the lining of the small intestine (Cleveland Clinic, 2022). This reaction prevents the absorption of essential nutrients, leading to a range of health issues.
Why Does Celiac Disease Occur?
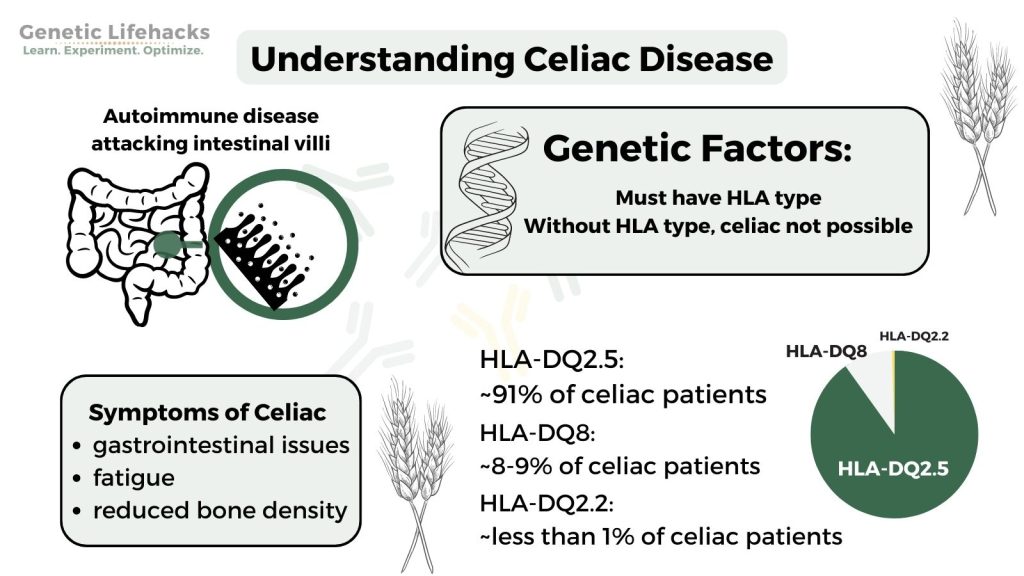
Celiac disease can occur at any stage of life, from infancy to adulthood. People with celiac disease have certain genetic markers, known as HLA-DQ2 and HLA-DQ8, which make them more likely to develop the disease (Cleveland Clinic, 2022). However, having these genetic markers does not mean a person will develop celiac disease.
The development of celiac disease involves a combination of genetic and environmental factors. A combination of factors such as stress, infection, surgery, or even hormonal changes, paired with the HLA-DQ2 and HLA-DQ8 genetic markers, can trigger the onset of celiac disease (Cleveland Clinic, 2022).
Common Symptoms
Celiac disease presents a variety of symptoms, which can range in severity and affect multiple body systems. Common symptoms that Cleveland Clinic (2022) highlight include:

- Gastrointestinal: Diarrhea, constipation, bloating, abdominal pain, and vomiting
- Nutritional deficiencies: Anemia, fatigue, weight loss, and bone weakness due to poor nutrient absorption
- Dermatological symptoms: a skin rash with blisters that appears on both sides of the body called Dermatitis Herpetiformis
- Neurological symptoms: Headaches, migraines, neuropathy, and cognitive impairment
- Growth and developmental delays: short stature, delayed and or irregular menstruation
Asymptomatic Celiac: Some individuals with celiac disease do not show the typical symptoms. Despite the absence of symptoms, the immune system still attacks the small intestine when gluten is consumed, causing damage that can lead to other health issues over time (Dennis, 2022). Even if an individual feels fine, untreated silent celiac disease can lead to long-term issues such as nutrient deficiencies, osteoporosis, or other autoimmune disorders
How Do You Get Tested?
Testing for celiac disease typically occurs in two phases:
Blood Tests are the first step in diagnosing celiac disease. They are used to detect specific antibodies, the most common being the tissue transglutaminase immunoglobulin A (tTG-IgA) test. Before using the tTG-IgA test, healthcare providers should determine if the person has an immunoglobulin A (IgA) deficiency, which is more common in people with celiac disease (Lehman, 2021). The healthcare provider can check for IgA deficiency by testing an individual’s IgA antibodies level.
If the individual is IgA deficient, relying only on the tTG-IgA test to diagnose celiac disease can lead to a false negative result. In these cases, other tests, like the immunoglobulin G (IgG) deamidated gliadin peptide (DGP) test, the IgG tissue transglutaminase (tTG) antibody test, or the IgG anti-endomysial antibody (EMA) test can be used to accurately diagnose celiac disease (Lehman, 2021).
For individuals with an increased risk of celiac disease, like those with Turner syndrome, regular blood tests may be recommended to screen for celiac disease even if the individual does not have symptoms.

Biopsy: If blood test results suggest celiac disease, a small intestinal biopsy is performed to confirm the diagnosis (Cleveland Clinic, 2022). This procedure looks for damage to the villi: tiny projections that absorb nutrients on the inside of the small intestine. In individuals with celiac disease, these villi are often flattened as a result of the immune system attacking the small intestinal lining (Cleveland Clinic, 2022).
Celiac Disease and Turner Syndrome
Individuals with Turner syndrome, a genetic condition characterized by the complete or partial absence of one X chromosome, have a higher risk of developing celiac disease than the average person (Mårild et al., 2016). This is likely because individuals with TS are generally more prone to autoimmune conditions (Mortensen et al., 2009). According to Bakalov et al. (2012), this increased risk of developing autoimmune conditions may be linked to missing parts of the X chromosome and hormonal imbalances caused by underdeveloped ovaries in individuals with TS.
Many individuals with Turner syndrome already face growth and hormonal challenges. If celiac disease goes undiagnosed, it can worsen issues like short stature, delay menstruation, and make growth hormone treatments less effective (Bonamico et al., 2002). Therefore, for those with Turner syndrome, who are known to be at a higher risk for celiac disease, screening is a proactive way to address potential causes of growth and hormonal problems.
Are There Treatments?
The main treatment for celiac disease is a lifelong gluten-free diet. Removing gluten from the diet allows the intestinal lining to heal and prevents further damage (Cleveland Clinic, 2022). Although sticking to a gluten-free diet can be challenging, it is crucial because even small amounts of gluten can trigger the body to attack itself again.
That being said, avoiding gluten is a significant lifestyle change, and it is important for people with celiac disease to be patient with themselves. Not following a strict gluten-free diet risks chronic inflammation in the small intestine, which can affect the entire body (Cleveland Clinic, 2022). After starting a gluten-free diet, it may take weeks, months, or even longer to start feeling better and for the small intestine to heal.
As for the diet itself, it can be discouraging going to buy groceries and feeling like there’s nothing you can eat. But keep your hopes up because with the increasing amounts of awareness for celiac disease, there are more and more alternatives available these days. Plus, many videos and online websites offer gluten-free recipe suggestions, such as this one.
Regular check-ups with healthcare providers, nutritional counseling, and monitoring symptoms are also essential parts of managing the condition. As more research is conducted on celiac disease, there is growing hope for new treatments and, hopefully, a cure in the future.

Key Takeaways
Celiac disease is an autoimmune disorder where eating gluten triggers an autoimmune response that damages the small intestine. Symptoms of this condition can affect many parts of the body.
Individuals with Turner syndrome are at a higher risk of developing celiac disease, so proactive screening is important for improving health outcomes.
Early diagnosis and a strict gluten-free diet are essential for managing symptoms and avoiding long-term health issues.
September 13, National Celiac Awareness Day, highlights the importance of raising awareness, supporting those with celiac disease, and promoting early diagnosis and treatment. This awareness and education allows us to have the many gluten-free options we have today.
If you or someone you know has symptoms of celiac disease, consult a primary care provider for proper testing and specialist referrals.
For even more information on TS and celiac disease, click here.
References:
Bakalov, V. K., Gutin, L., Cheng, C. M., Zhou, J., Sheth, P., Shah, K., Arepalli, S., Vanderhoof, V., Nelson, L. M., & Bondy, C. A. (2012). Autoimmune Disorders in Women with Turner Syndrome and Women with Karyotypically Normal Primary Ovarian Insufficiency. Journal of Autoimmunity, 38(4), 315–321. https://doi.org/10.1016/j.jaut.2012.01.015
Bonamico, M., Pasquino, A. M., Mariani, P., Danesi, H. M., Culasso, F., Mazzanti, L., Petri, A., & Bona, G. (2002). Prevalence and Clinical Picture of Celiac Disease in Turner Syndrome. The Journal of Clinical Endocrinology & Metabolism, 87(12), 5495–5498. https://doi.org/10.1210/jc.2002-020855
Cleveland Clinic. (2022, December 12). Celiac disease. https://my.clevelandclinic.org/health/diseases/14240-celiac-disease
Dennis M.(2022, October 11). Silent celiac disease. National Celiac Association. https://nationalceliac.org/celiac-disease-questions/silent-celiac-disease
Lehman, J. (2021, March). Serologic testing for celiac disease in patients with IgA deficiency. [Presentation Transcription]. Mayo Clinic Laboratories. https://news.mayocliniclabs.com/2021/03/11/serologic-testing-for-celiac-disease-in-patients-with-iga-deficiency
Mårild, K., Størdal, K., Hagman, A., & Ludvigsson, J. F. (2016). Turner syndrome and celiac disease: A case-control study. Pediatrics, 137(2). https://doi.org/10.1542/peds.2015-2232
Mortensen, K. H., Cleemann, L., Hjerrild, B. E., Nexo, E., Locht, H., Jeppesen, E. M., & Gravholt, C. H. (2009). Increased prevalence of autoimmunity in Turner syndrome – influence of age. Clinical and Experimental Immunology, 156(2), 205–210. https://doi.org/10.1111/j.1365-2249.2009.03895.x
Turner Syndrome Foundation. (2024). Celiac. https://turnersyndromefoundation.org/what_is_turner_syndrome/autoimmune-diseases/celiac
Written and Researched by Victoria Brown, TSF volunteer blog writer. Edited and Designed by Riya Ajmera, TSF Blog Coordinator. Peer-Reviewed by Mary Gwyn Roper, MD and Kayla Ganger, PA-C. Cover Graphic by Riya Ajmera.
© Turner Syndrome Foundation, 2024





